
As one of the largest metabolic and bariatric surgery centers in the world,
Kaiser Permanente Southern California sought to reimagine how it prepared and supported its patients every step of their journey. Kelly Dumke, DrPH, Senior Learning Consultant from Kaiser Permanente’s Center for Healthy Living presented their Human Centered Design process insights at MadPow’s Health Experience Design Conference HxD 2021 within the Person- Centered Care Experiences track.
5 Questions in 5 mins, Interview by Sherri Dorfman, MBA, CEO Stepping Stone Partners
Q1. As a “non-designer”, how did you learn to approach this member program through a new lens?
A1. At the very beginning of this initiative, the Human Centered Design (HCD) at Kaiser Permanente Training taught me how to use the core tools and practices of human centered design and also gave me coaching as I learned to apply it. Their model of both practicing HCD and spreading the mindset and methods throughout Kaiser Permanente is truly inspiring. Overall, human centered design empowered me to embrace designing WITH patients (and not just for them) and it makes my job more fun and (hopefully) much more impactful.
Q2. You mentioned working with your clinicians to identify patients either going through or considering going through the bariatric program. Your data indicated that there were disparities in outcomes. How did you capture insights from patients who were not successful?
A2. Our clinicians gave us names of many patients who had gone through our program, but we found that those who were willing to talk and join our codesign sessions were typically successful with the surgery. We were not getting the perspective of those who were not as successful or struggled along the journey. We realized that we needed to do a set of ethnographic interviews to understand their specific situations to uncover barriers. We also interviewed caregivers to gain insight into their support system.
Q3. What was the biggest surprise that your team uncovered about these bariatric patients during the “Understand Phase”?
A3. We had a patient tell us “I had surgery on my stomach, not on my mind”. We realized how important it was to design this program not only to prepare a patient, but to address and support their mental and emotional health before and after the surgery. Many patients also disclosed experiences with trauma in the past that may play into maladaptive coping mechanisms that contributed to weight gain.
Q4 While imagining solutions for your patients, you invited the staff to be join the process. How did their perspective enhance the design process?
A4. We invited our staff to observe the patient’s co-design to hear needs firsthand. Then we asked the staff to participate in a co-design session and brainstorm solutions and ideas together with patients. For example, one operational issue that surfaced was that some patients did not even feel comfortable coming into our medical centers that didn’t have furniture that could accommodate different body types. Together, we explored solutions such as larger more comfortable chairs for patients in the waiting area.
Q5. How did your project team use the patient centered design insights to build a stronger understanding between patients and providers?
A5. During workshops, we devised eleven personas to define different reasons why patients were in the program such as losing weight to get other surgeries or improving their health. By sharing these profiles with the staff, we helped them better understand the differences in patient motivations for the surgery. We also created a top 10 list of what patients want you to know up front when considering surgery, which enables the staff to more effectively set expectations with patients at the start of the program.
Notice how Kaiser Permanente has co-created with patients and staff to design a better care experience at every journey step, across different channels, from in- person appointments to digital patient education tools.
 Permalink
Permalink  April 27, 2021
April 27, 2021 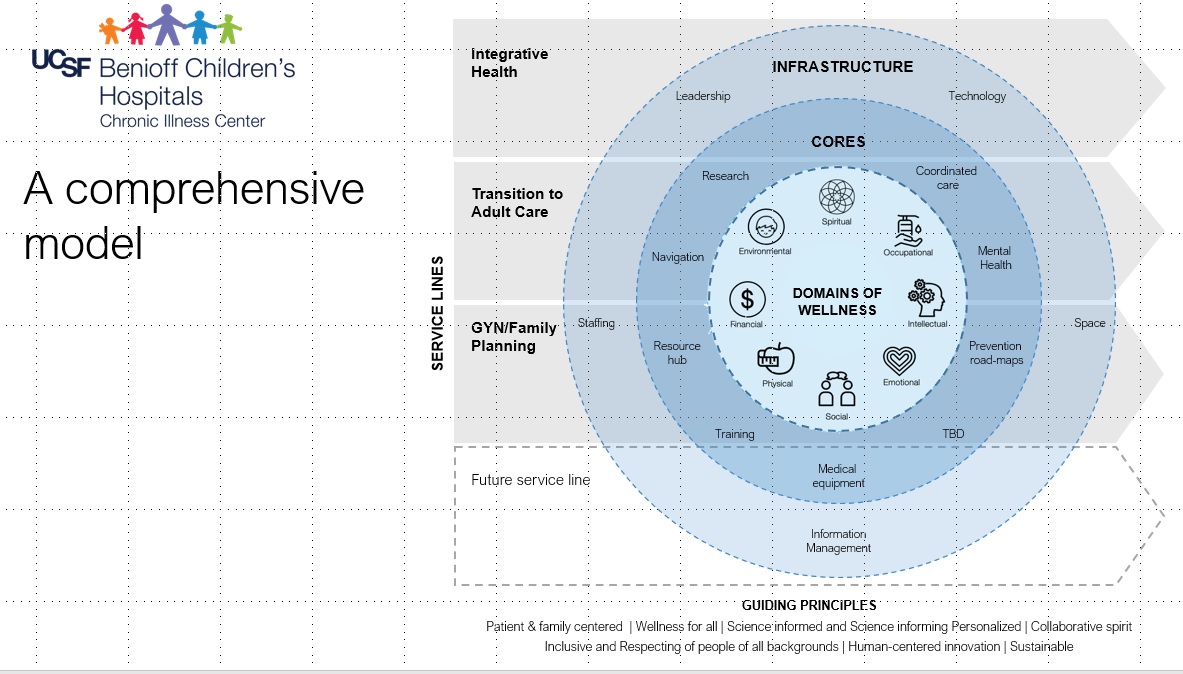 The journey for pediatric patients with multiple co-morbidities can be complex, with some patients receiving care from 20+ providers. Jan Yeager, Service Designer, UCSF shared experiences co-designing a Chronic Illness Center with patients, caregivers, UCSF physicians and clinicians, and community providers at MadPow’s 2021 Health Experience Design Conference.
The journey for pediatric patients with multiple co-morbidities can be complex, with some patients receiving care from 20+ providers. Jan Yeager, Service Designer, UCSF shared experiences co-designing a Chronic Illness Center with patients, caregivers, UCSF physicians and clinicians, and community providers at MadPow’s 2021 Health Experience Design Conference. April 26, 2021
April 26, 2021  As one of the largest metabolic and bariatric surgery centers in the world, Kaiser Permanente Southern California sought to reimagine how it prepared and supported its patients every step of their journey. Kelly Dumke, DrPH, Senior Learning Consultant from Kaiser Permanente’s Center for Healthy Living presented their Human Centered Design process insights at MadPow’s Health Experience Design Conference HxD 2021 within the Person- Centered Care Experiences track.
As one of the largest metabolic and bariatric surgery centers in the world, Kaiser Permanente Southern California sought to reimagine how it prepared and supported its patients every step of their journey. Kelly Dumke, DrPH, Senior Learning Consultant from Kaiser Permanente’s Center for Healthy Living presented their Human Centered Design process insights at MadPow’s Health Experience Design Conference HxD 2021 within the Person- Centered Care Experiences track.

